%20(1).png)
April 10, 2026
The 2026 mandate for Ontario Health Teams (OHTs) is clear: attach an additional 500,000 patients to primary care teams. While the goal is ambitious, the path forward is often obstructed by fragmented data and technical silos that leave over 10% of the population in many OHT regions unattached.
On March 31, 2026, IDENTOS, Amplify Care, and Empower Health hosted a strategic webinar to address this challenge. The session explored how interoperable infrastructure can reduce the "digital friction" caused by multiple logins and slow system access—the top digital barriers currently faced by Ontario GPs.
To kick off the session, we polled our attendees on the biggest roadblocks they face when trying to attach patients in their local communities.
A live poll of over 130 attendees revealed a fragmented landscape of challenges:
These results confirm that attachment isn't just a human resource problem; it is a data and coordination problem.
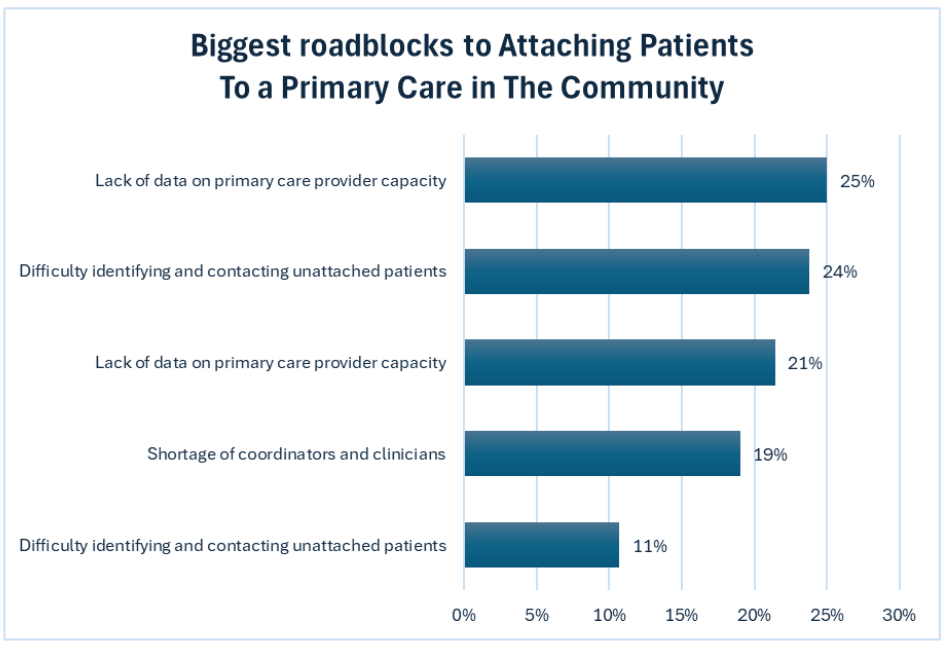
Even when capacity exists, a technical "invisible barrier" prevents it from being utilized efficiently.
According to the 2024 National Survey of Canadian Physicians by Canada Health Infoway, the infrastructure itself is often the enemy of productivity:
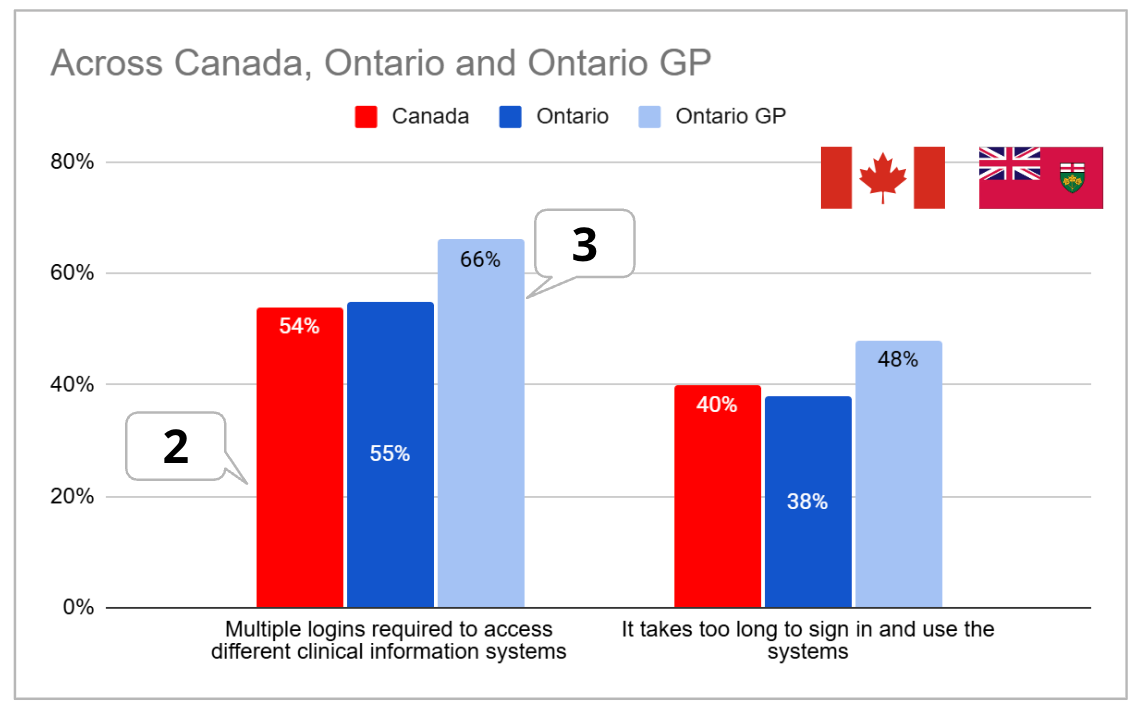
For an Ontario GP, digital friction is the third biggest barrier to providing care. If we want clinicians to take on more patients, we must first reduce their administrative load.
IDENTOS, Amplify Care and Empower Health propose a combined scalable attachment solution utilizing the strengths of all three partners to streamline the attachment process.
In this ecosystem, IDENTOS provides the "trust exchange" layer (the DTX), while Empower provides the high-fidelity data layer, and Amplify provides the change management expertise.
Ryan Doherty (Founder, Empower Health) explains the necessity of a "governed data layer". Unlike provincial data that may include retired physicians or home addresses, Empower’s directory provides real-time, validated information on:
IDENTOS provides the Digital Health Trust Exchange (DTx), the core infrastructure of this integrated solution. By leveraging this exchange and the Health Application Lightweight Protocol (HALO), clinicians can launch necessary tools directly from their EMR using Single Sign-On (SSO)—eliminating the need for yet another set of credentials.
Ted Alexander (VP Partnership, Amplify Care) emphasizes that technology alone isn't enough. Amplify Care focuses on "Practice Facilitation" - working on the ground to align digital tools with the actual workflows of interprofessional care teams to meet the Quintuple Aim.
One of the most compelling segments showcased how high-fidelity data enables GIS (Geographic Information System) mapping.
A final poll during our session revealed a significant knowledge gap in the industry.
Insight: 56% of attendees reported being "Unaware" of HALO standards.
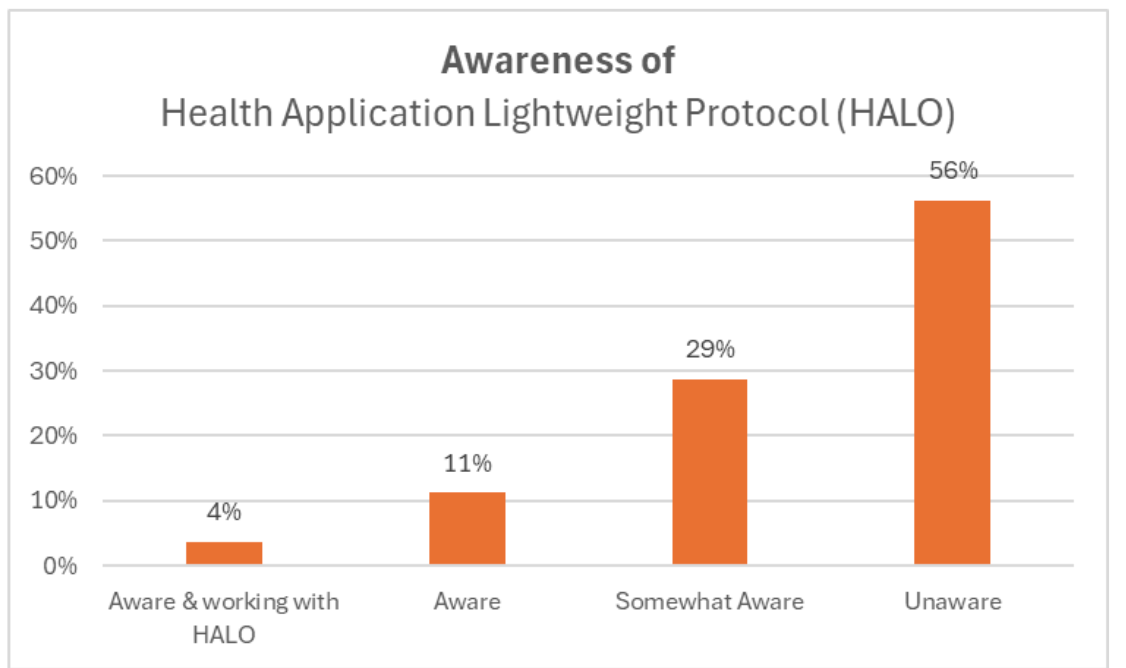
As Ontario pushes toward more integrated care, understanding these standards will be the difference between scalable success and technical debt.
Scaling patient attachment is a community effort that requires aligning technology with clinical workflow. IDENTOS, Empower, and Amplify are hosting a series of Co-design Workshops over the next three months to help OHTs and PCNs implement these solutions.
These sessions will help bridge the gap between high-level provincial goals and the day-to-day realities of community clinics.
Interested in joining a workshop? Contact us here to get started.
This post is a recap of the "Scaling Patient Attachment for Ontario Health Regions" webinar. For the full recording and slide deck, click here.
If you have any questions or require further information regarding this topic, please don’t hesitate to contact us using the form below.




